What is presbyopia, and what are corneal inlays for?
The KAMRA small aperture corneal inlay is an implant that corrects presbyopia by improving the near vision in patients who are older than 45 years of age. Presbyopia is the age-related inability of the human eye to “autofocus” for near, due to the weakening of the muscles of the eye’s natural lens. It is most prominent after the age of 40. People then have to wear glasses to read the time off their watch, to read and write messages on mobile phones, read newspapers, and work on computers. Candidates for the KAMRA inlay are patients 45 years of age or older, who are motivated and want to have minimal dependency, if any, on eyeglasses for both far and near. [view photos]
The KAMRA inlay procedure can be performed on its own, or combined with LASIK in one or two sessions in patients who suffer also from visual errors for far, like myopia (near-sightedness), hyperopia (far-sightedness), or astigmatism. The LASIK procedure fixes the far, and the KAMRA implant fixes the near. In patients with no visual errors for far, a pocket is created in the cornea, the outer transparent portion of the eye, using a specialized laser called femtosecond laser. The KAMRA inlay is then inserted into the pocket and centered over the pupil and the visual axis. In patients with visual errors for far, like myopia, hyperopia, or astigmatism, a LASIK procedure is performed to correct the visual error: A small flap is created in the front portion of the cornea using the femtosecond laser, then small laser bubbles are created and the surgeon later connects them, hence creating a flap. The flap is then lifted, and an excimer laser controlled by a computer then sculpts the cornea, changing its curvature to better focus light on the retina. Thereafter, the KAMRA corneal inlay is inserted into the cornea through a laser created pocket underneath the corneal flap. The KAMRA inlay is positioned over the pupil, around the visual axis. The exact location of the inlay is guided by state-of-the-art measurements and guidance technologies performed before as well as during the procedure. The KAMRA surgery is quick and is performed while the patient is awake in an outpatient setting under local anesthesia using numbing eye drops. The KAMRA inlay is performed in only one eye, the non-dominant eye, which is determined before surgery. The eye with the KAMRA inlay might see a little less than the fellow eye for far, but this is minimal, and is not noticeable with both eyes open. On the other hand, the eye with the KAMRA inlay will be much better for near. Vision for near with both eyes open improves markedly as driven by one eye, while vision for far is kept or made excellent in either eye. [view photos]
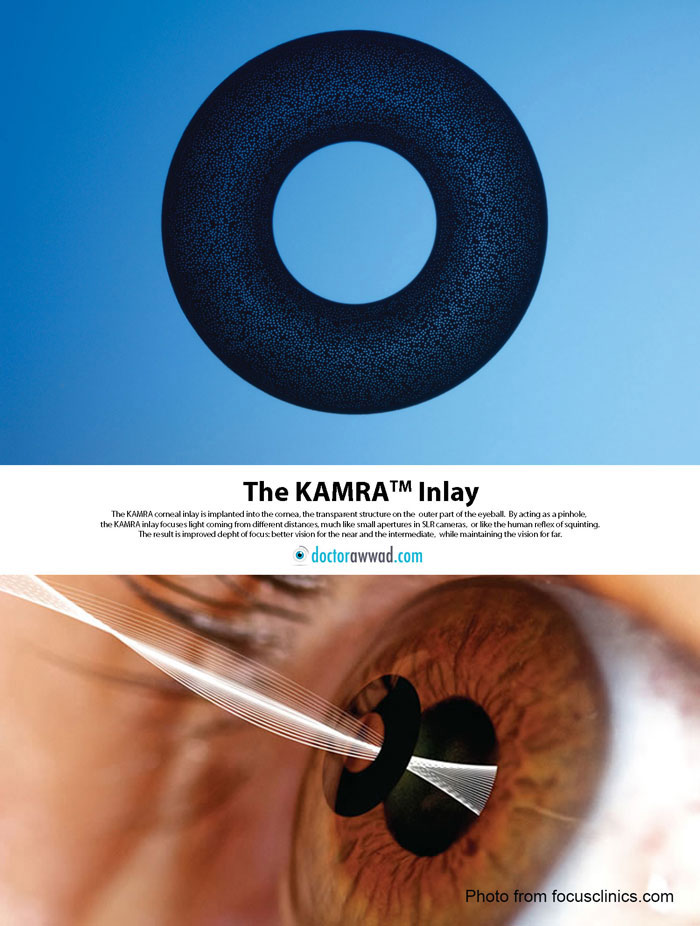
When normal individuals want to see better, they “squint”, meaning they bring their eyelids close to each others to see better. By doing so, people filter out the peripheral rays of light and allow only the central ones to enter. The central rays of light allow better vision over a larger distance range, resulting in a better depth of focus. Professional single light reflex or SLR cameras use the same concept by allowing photographers to control the width of the lens aperture. Smaller apertures allow larger depth of focus, with objects at different distances all looking sharp, while larger apertures bring objects positioned at a certain distance into focus, while objects at other distances would look blurred. The KAMRA inlay make use of the same physical principle: it has a 1.6 mm central hole which filters the peripheral light rays and allows the central rays to enter the eye, hence increasing the depth of focus and simulating squinting: objects at different distances from the human eye come into focus: the near, the intermediate, and the far. The action of the KAMRA inlay is independent of the accommodation of the human eye, and hence, its effect remains stable and does not weaken over time.
In patients with concomitant myopia, hyperopia, or astigmatism, vision for far improves starting the next day after the procedure, with further improvement over several weeks. Patient can usually drive the next day. Near vision improves over several weeks to several months, but many patients notice a great deal of improvement in the first few days after the procedure. Around 4% of patients might need a small procedure in the first few weeks postoperatively to adjust the position of the corneal inlay. Just like LASIK, patients will experience dry eyes for up to 6 months and sometimes more. Dry eyes can lead to visual fluctuation, especially for near vision; patients will need to use lubricant drops, which will improve vision, especially for near. With time, brain adaptation as well as decrease in dryness will dramatically improve near vision and make it more robust and constant. Studies around the world have shown that around 90% of patients will be able to read newspapers and send text messages on their cell phones without eyeglasses. The rest will still be able to perform many close-up activities without spectacles, and hence, would be less dependent on eyeglasses. Around 1-2% of the inlays might need to be explanted for many benign reasons, like no appreciable improvement for near, haloes at night, or unsatisfactory vision for far. The KAMRA inlay procedure can be combined with LASIK if a patient suffers from visual errors for far. It improves the near vision without appreciably affecting the far vision. Its effect is stable and does not wane over time, resisting the progressive nature of presbyopia. The procedure is performed in only one eye, the non-dominant eye, sparing the dominant one, and it is completely reversible, as the inlay can be removed from the cornea at any time without any problem, even years later.